Dental Implant Specialist
Offering Life-Changing Dental Implants
Dental Implant Specialist
Offering Life-Changing Dental Implants
Dental Implant Specialist
Offering Life-Changing Dental Implants
Dr. E. Richard Hughes
A DENTAL IMPLANT SPECIALIST and Comprehensive Dentist
Dr. E. Richard Hughes has been practicing dentistry in Sterling, VA for over three decades. Since founding his practice in 1987, Dr. Hughes’s extensive training and dedication to individualized care have earned him an excellent reputation as the preferred dentist for dental implants in Sterling, Reston, Ashburn, and other communities throughout Loudoun County, VA.
Dr. Hughes has a number of impressive credentials and memberships. He is one of only 500 dentists to receive the distinction of Diplomate with the American Board of Oral Implantology. Additionally, he is:
- Board Examiner, American Board of Oral Implantology
- Board Member & Fellow, American Academy of Implant Dentistry
- Fellow, American Academy of Implant Prosthodontics
Dr. Hughes has appeared as a guest, lecturer, and consultant on implant dentistry for various national and international media outlets. He has also testified before the Food and Drug Administration for the reclassification of Blade Implants, a type of dental implants.

Dr. Richad Hughes
Dr. Hughes Is a Top Implantologist
He Can Restore Your Smile with Dental Implants
If you are missing teeth, consider restoring your smile with state-of-the-art dental implants. Implants are threaded titanium posts designed to replace tooth roots and prevent bone recession after tooth loss. Depending on how many teeth you are missing, they can support dental crowns, dental bridges, and dentures.
Looking for dental implants in Sterling VA? Contact Dr. Hughes’ dental office. He has been placing implants for over 20 years and is an authority in the field of implant dentistry in Sterling, VA. He uses the latest materials and advanced technology to help patients experience the many benefits of implants. These include…
Natural Look and Feel
Our dentist custom designs implant-supported restorations to match the color, size, and shape of your natural teeth. Implant-supported restorations are permanently attached to your implants, so they will look and feel like a natural part of your smile.
Maximum Stability and Longevity
Implants secure crowns, bridges, and dentures to the jawbone, so your restoration will stay put while you speak and chew. While your implant-supported restoration will need to be replaced every ten years or so, the titanium posts themselves can last a lifetime.
Better Oral Health
Dental implants are the only dental treatment designed to stop bone loss. Just like tooth roots, these titanium posts stimulate the jawbone, prevent bone recession, and keep your jawline intact.
Prepare for Your Visit
To help the dentist and staff get to know you before your appointment, we encourage you to download, print, and fill out our patient forms.
Patient Information | Medical History
Implant Questionnaire | Sleep Apnea Questionnaire
We Put Patients First
Discover What Our Practice Is All About…
Listen as Dr. Hughes describes his approach to dentistry, dental implants and patient-focused dental care…
Wybierz spośród szerokiej gamy gier w pokera wideo. Walcz z domem o najlepszy układ pięciu kart. Potasuj karty i wygraj dużą sumę. Już wkrótce na portalu TopKasynoOnline znajdziesz autentyczne wrażenia z gry w kasynie online. Wejdź w interakcję z prawdziwymi krupierami w różnych grach, takich jak blackjack na żywo, ruletka na żywo, bakarat na żywo i wiele innych. Gry z krupierem na żywo będą przesyłane bezpośrednio na Twój ekran w czasie rzeczywistym! Nieważne czy jesteś amatorem czy doświadczonym graczem, na Top-Kasyno-Online Polska topkasynoonline.com zawsze znajdziesz najnowsze wersje gier. Gry kasynowe online takie jak video sloty, blackjack, ruletka i wiele innych znajdziesz tutaj, aby grać dla zabawy! Ponieważ świat gier online jest jedną z najbardziej konkurencyjnych dziedzin, twórcy oprogramowania zawsze ścigają się w tworzeniu najlepszych gier na rynku. Na portalu Top Kasyno Online PL dbamy o to, aby zawsze być na bieżąco z nowościami, więc możesz je wypróbować za darmo!
Become a Part of the Family
Schedule a Consultation with Our Dentist


From routine dental exams to advanced restorative dentistry, your entire family can benefit from our high-quality care and life-changing results.
For Dr. Hughes, dentistry is more than a profession. Dr. Hughes knew dentistry was his calling at a young age after watching his grandfather help others as a dentist. He finds the profession highly rewarding and strives to treat everyone with the same level of personalized care. Dr. Hughes’s patients appreciate his thorough, compassionate approach and continually return to our practice for their dental needs.
Are you ready to experience a higher quality of care for your dental implants? You can schedule an appointment at our Sterling, VA, office today by contacting us online or calling:
(703) 444-1152
Comprehensive Dental Care in a Comfortable, Modern Office
Improve the Look of Your Smile
Restore the Health of Your Smile
- Restorative Dentistry Overview
- Dental Implants
- All-on-4®
- Dental Implant Surgery
- Cost of Dental Implants
- Benefits and Risks of Dental Implants
- Dental Implant Candidate
- Dental Implant FAQs
- Dental Fillings
- Dental Bridges
- Dentures
- Implant-Supported Dentures
- Inlays and Onlays
- Full Mouth Reconstruction
- Dental Crowns
- Bone Grafting
- Scaling and Root Planing
Our Mission
To Provide A Superior Dental Experience
Committed to Your Comfort
Dr. Hughes understands that dental anxiety is a very real obstacle for some people. To help you overcome your fears and achieve optimal health, he offers:
Sedation Options
We offer effective oral sedation and nitrous oxide to help you achieve maximum comfort throughout the duration of your dental appointment.
Comforting Environment
Our cozy office is complete with headphones, magazines, and other amenities to keep you entertained during your visit.
Precise Approach
Due to our years of experience and our gentle approach, most patients experience very little or no discomfort at all during dental procedures.
Five Stars!
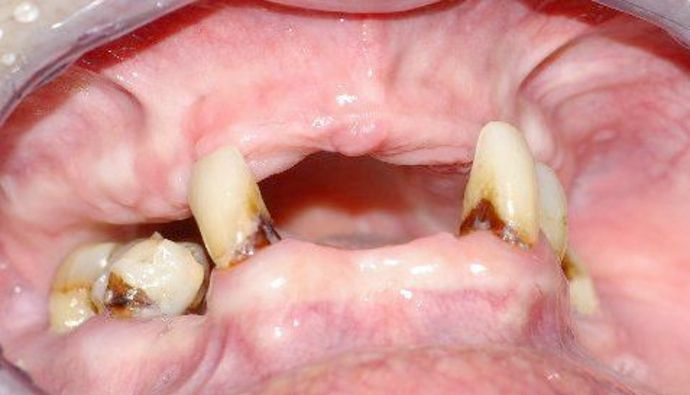
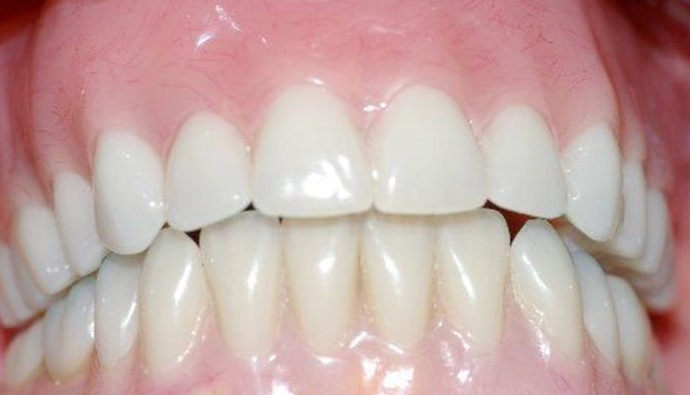
Implants Can Make a Dramatic Difference View One of Our before & after Cases
View One of Our before & after Cases
This patient came to our Sterling, VA, practice with widespread tooth loss. Our dentist treated this individual with custom-designed implant-supported dentures.
Flexible Payment Options
We Work with Your Budget
Credit Cards
We accept most major credit card including Visa, MasterCard, Discover,and American Express.
Patient Financing
We work with your financial situation and can arrange an in-house payment plan that suits your needs and budget.